

Evidence-informed dental care for enhancing smile brightness while safeguarding long-term oral health
Tooth whitening represents a responsible, evidence-informed approach to enhancing smile brightness while safeguarding long-term oral health. In the United Kingdom, professional tooth whitening is recognised as a clinical dental procedure rather than a purely cosmetic treatment. It involves the controlled use of peroxide-based whitening agents that penetrate the enamel surface and break down stain molecules within the tooth structure.
This chemical process lightens intrinsic and extrinsic discolouration without mechanically removing enamel, ensuring that the natural tooth surface remains intact when treatment is carried out correctly. Before any whitening procedure begins, a thorough dental assessment is essential. A qualified dental professional evaluates the condition of the teeth and gums, checks for decay, gum disease, enamel wear, cracks, and the presence of restorations such as crowns, veneers, or fillings.
This assessment ensures suitability and helps determine the most appropriate whitening method. Supervised treatment reduces the risk of complications such as uneven shade results, gum irritation, or heightened tooth sensitivity. Protective measures are carefully used to shield soft tissues, and whitening concentrations are selected within legal and clinical safety limits.
The goal of professional tooth whitening is not to create an artificial or opaque appearance. Instead, the intention is to achieve a balanced, natural-looking improvement in shade that complements facial features and maintains authenticity. Responsible whitening respects the structural integrity of enamel and acknowledges that existing restorations will not change colour. Where necessary, treatment planning may include advice on replacing visible restorations after whitening to ensure uniform aesthetics.

Smile brightness plays a meaningful role in how individuals perceive themselves and how others perceive them. A brighter smile is often associated with vitality, attentiveness, and self-care. For many people, whitening treatment becomes a catalyst for renewed confidence in professional, social, and personal settings. Feeling comfortable when speaking, laughing, or appearing in photographs can positively influence daily interactions and overall self-esteem.
Beyond appearance alone, the decision to pursue tooth whitening often encourages improved oral hygiene habits. Individuals may become more mindful of brushing technique, flossing routines, and regular dental visits. It can also motivate lifestyle changes such as reducing tobacco use or limiting consumption of staining beverages like coffee, tea, and red wine. In this way, whitening becomes part of a broader commitment to preventive oral care rather than an isolated cosmetic step.
When approached responsibly, professional tooth whitening supports both aesthetic enhancement and long-term dental health. It reinforces the importance of professional supervision, ethical standards, and realistic expectations. A brighter smile, achieved through clinically guided care, reflects not only improved shade but also a sustained dedication to oral wellbeing and overall confidence.
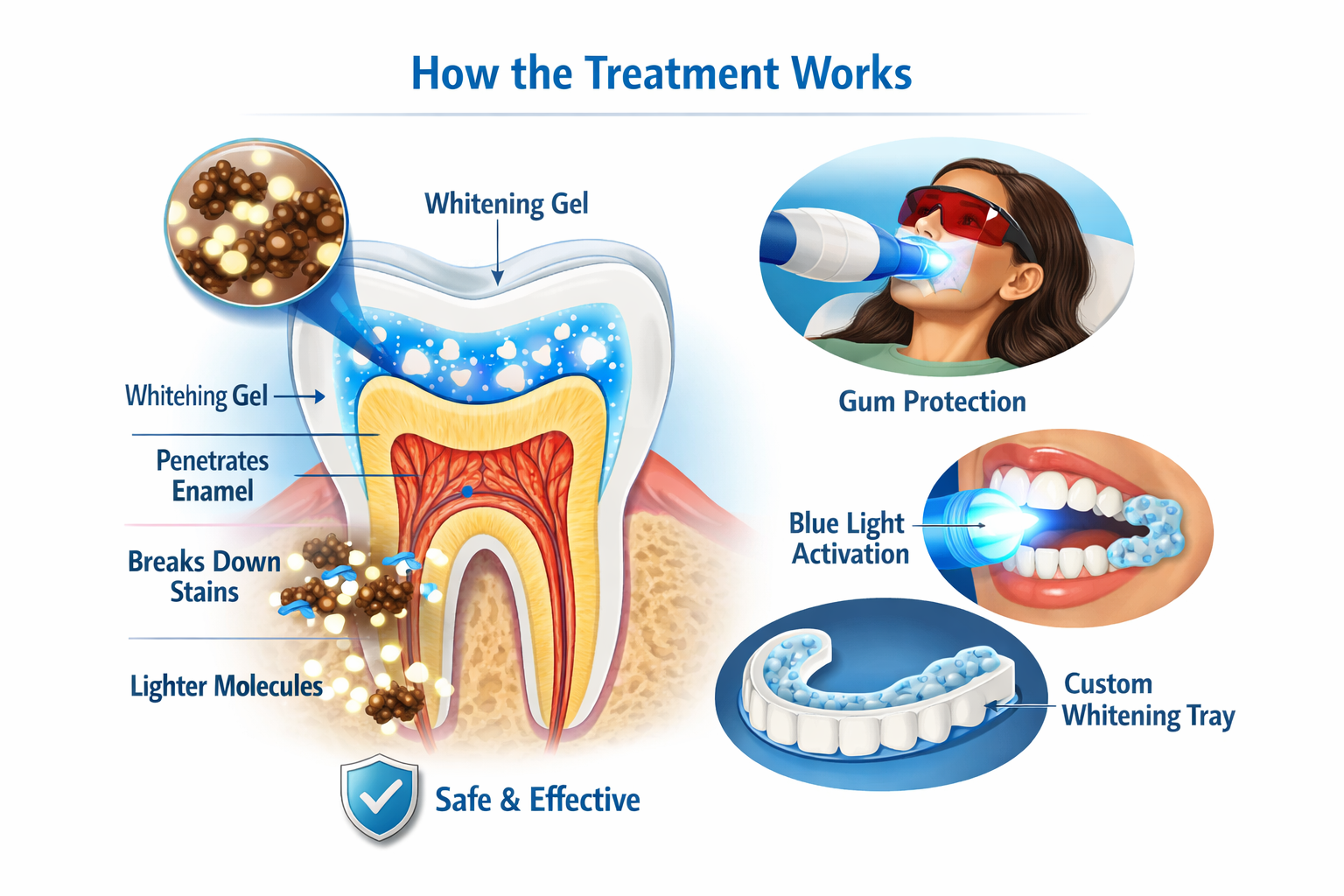
Professional tooth whitening uses peroxide-based agents that work at a molecular level to break down stain molecules within the tooth structure. The whitening gel penetrates through the enamel surface, reaching the deeper layers where discolouration has accumulated over time. This chemical reaction transforms stain molecules into smaller, lighter-coloured compounds, resulting in a brighter appearance.
The process does not mechanically remove or damage the enamel when performed correctly under professional supervision. Instead, it chemically alters the colour of the tooth's internal structure while preserving the natural tooth surface. The concentration of the whitening agent, the duration of application, and the method of delivery are all carefully controlled to ensure both safety and effectiveness.
During professional treatment, protective measures are implemented to shield the gums and soft tissues from contact with the whitening gel. Custom-fitted trays or barrier materials ensure that the active ingredients remain in contact with the tooth surfaces while minimising exposure to surrounding tissues. This precision is a fundamental distinction between professional treatment and over-the-counter products.

Not everyone is an immediate candidate for tooth whitening. A comprehensive clinical assessment determines suitability by evaluating multiple factors. The condition of the teeth and gums, the presence of dental restorations, enamel thickness, and individual sensitivity levels all influence whether whitening is appropriate and which approach would be most effective.
Individuals with healthy teeth and gums, minimal restorations in visible areas, and realistic expectations tend to achieve the most satisfactory results. Those with extensive crowns, veneers, or composite fillings in the smile zone may require additional planning, as these materials do not respond to whitening agents. In such cases, a discussion about potentially replacing restorations after whitening becomes an important part of treatment planning.
Certain conditions may temporarily or permanently contraindicate whitening. Active tooth decay, untreated gum disease, severe enamel erosion, or exposed dentine requires attention before any whitening procedure. Pregnant or breastfeeding individuals are generally advised to defer elective whitening as a precautionary measure. Similarly, those under 18 years of age are restricted from receiving treatments containing hydrogen peroxide at therapeutic levels, except in specific disease-related circumstances.
Pre-Treatment Assessment Includes:
Comprehensive oral examination to identify decay, gum disease, cracks, or other conditions that could be aggravated by whitening. Review of existing restorations and discussion of how final shade will relate to crowns, veneers, and fillings. Evaluation of past sensitivity and enamel status. Medical and medication history review. Age verification and regulatory compliance check. Informed discussion of realistic expectations using shade guides and photography.

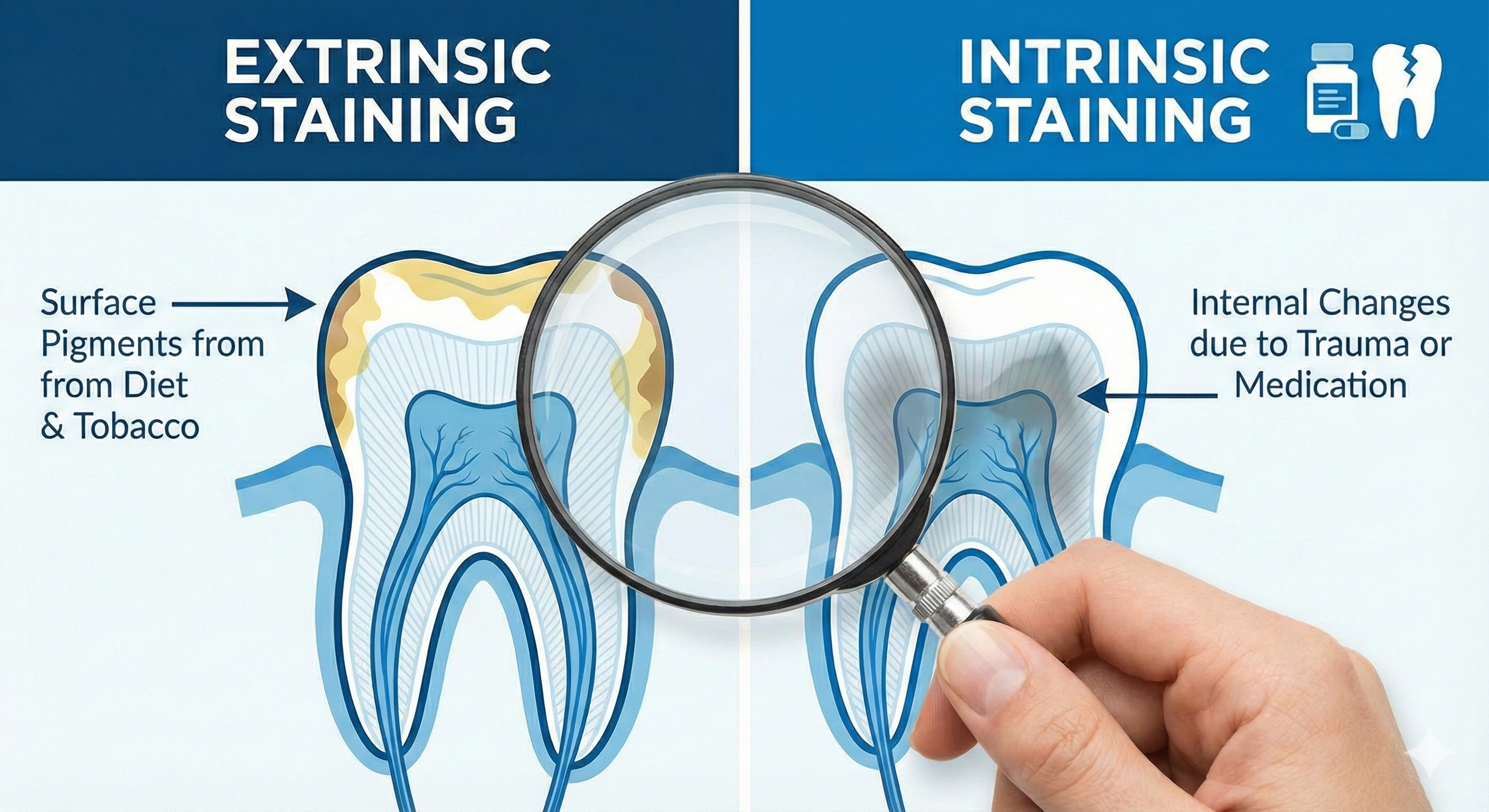
Teeth rarely change colour without reason. Discolouration is usually the result of gradual, everyday exposure to staining agents, natural biological changes, or specific medical and developmental influences. Understanding the underlying cause is essential before considering whitening treatment, as different types of staining respond differently to professional care. A clear diagnosis allows dental professionals to set realistic expectations and recommend the most appropriate approach.
Extrinsic staining affects the outer surface of the tooth, specifically the enamel. This type of discolouration develops when pigments from food, drink, or tobacco attach to the tooth surface. Common contributors include coffee, tea, red wine, fizzy drinks, richly coloured spices, and smoking. Over time, these pigments accumulate, especially if oral hygiene is inconsistent or professional cleaning is infrequent.
Surface stains often appear yellow, brown, or slightly grey. Because they sit on or near the enamel, they generally respond well to professional scaling, polishing, and regulated whitening treatments. However, even extrinsic stains can become more stubborn if they remain untreated for long periods, as they may penetrate slightly into microscopic enamel pores.
Intrinsic discolouration occurs within the tooth's internal structure, affecting the dentine or deeper enamel layers. This type of staining is typically more complex and may not respond as easily to standard whitening procedures. Common causes include exposure to tetracycline antibiotics during tooth development, excessive fluoride intake in early childhood (dental fluorosis), or trauma to a tooth that disrupts its internal blood supply.
When trauma occurs, the tooth may gradually darken due to changes in its internal tissues. Intrinsic stains often appear grey, blue, or deep brown and may require specialised treatment planning. In some cases, internal whitening techniques or restorative solutions may be considered instead of conventional external whitening.
As individuals age, natural structural changes in teeth contribute significantly to discolouration. Enamel, the outer protective layer, gradually thins over the years of chewing, brushing, and minor wear. As enamel thins, the underlying dentine, which is naturally more yellow, becomes more visible. At the same time, dentine itself can darken and become more saturated in colour over the years.
These combined changes often result in a duller or less vibrant smile. Age-related discolouration is typically a mixture of intrinsic and extrinsic factors, meaning treatment outcomes can vary depending on enamel thickness and overall tooth condition.
Dental restorations such as crowns, veneers, bonding, and composite fillings do not respond to peroxide-based whitening agents. This is an important consideration during treatment planning. If natural teeth are whitened but existing restorations remain unchanged, colour mismatches may become noticeable. For example, a crown placed years earlier to match a slightly darker tooth shade may appear comparatively darker after whitening.
A thorough pre-treatment assessment helps identify such risks, allowing for coordinated planning if replacement or adjustment of restorations is needed to maintain a balanced appearance.
Certain systemic illnesses, medications, and genetic conditions can influence tooth colour. Some metabolic disorders, enamel formation abnormalities, or prolonged medication use may cause unusual patterns of staining, including banding or uneven patches. These cases require careful clinical evaluation to determine whether whitening is suitable or if alternative cosmetic options would provide better results.
Professional tooth whitening encompasses several evidence-based approaches, each with specific advantages, limitations, and predictable patterns of response. The choice of method depends on individual circumstances, the nature of discolouration, time constraints, and personal preferences.
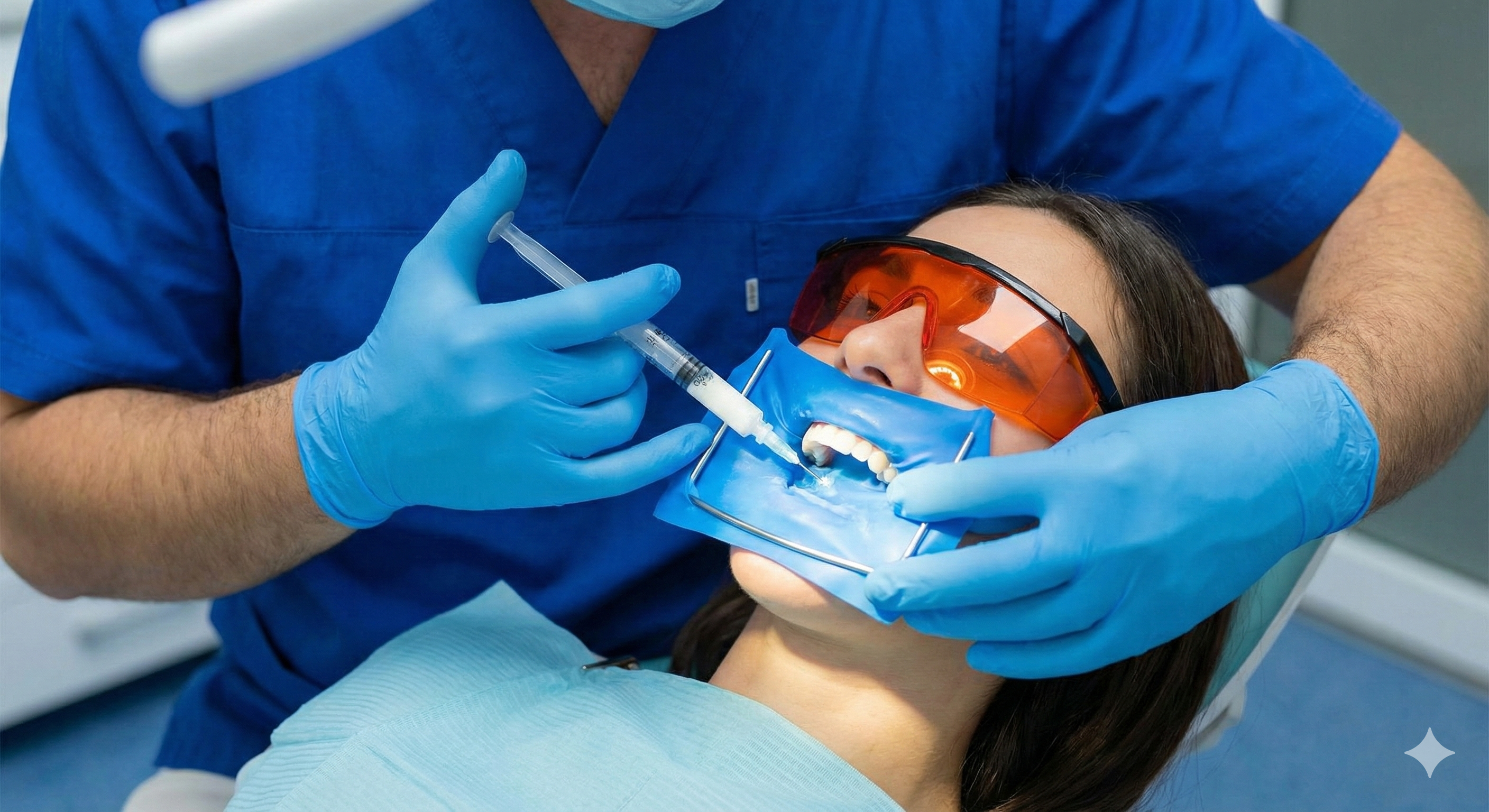
Performed in a dental clinic by a dentist or by a qualified dental team member under direct supervision, in-practice whitening typically uses higher-concentration peroxide gels applied to cleaned teeth. The procedure may involve rubber dam or gingival protection to shield soft tissues, controlled application of whitening gel in brief cycles often repeated in a single visit to achieve a noticeable change, and in some systems, use of light activation.
Although evidence supporting extra benefit from lights is mixed, clinicians may select systems based on established safety and efficacy. This approach offers immediate, measurable shade improvement after one session with possible short-term sensitivity that usually resolves. This option suits patients who want faster results under close supervision.
A commonly selected approach for gradual, controlled lightening involves custom-made trays fabricated from impressions or digital scans. A dental-strength bleaching gel within regulated peroxide limits is supplied along with detailed instructions. The patient wears the trays for prescribed periods, either overnight or during the day, across several days or weeks.
Advantages include excellent shade control, predictable outcomes, and the ability to titrate exposure to manage sensitivity. This method allows for a more gradual transformation and can be adjusted based on individual response and comfort levels.
Some clinicians combine an in-practice boost with a home tray programme. An initial chairside session produces an immediate lift, followed by tray use that refines and stabilises shade. This approach can be ideal for moderate to severe discolouration or for patients seeking quicker but long-lasting results. It combines the immediate gratification of in-office treatment with the controlled refinement of home-based care.
When a tooth darkens following trauma or root canal treatment, internal bleach can be placed within the tooth structure by a dentist. This is a distinct clinical procedure requiring specialist assessment and an understanding of long-term restorative needs. The whitening agent is placed inside the tooth chamber, allowing it to work from within over several days or weeks.
Low-strength over-the-counter products can offer minor cosmetic improvement for very superficial staining. However, they cannot match clinically prescribed systems and are no substitute for an assessment where restorations or intrinsic stains are present. For meaningful, safe whitening, clinician involvement is strongly recommended.
The degree of improvement achievable through tooth whitening varies considerably depending on the type and severity of discolouration, the whitening method selected, and individual biological factors. Professional treatment aims for natural-looking enhancement rather than an artificially bright or uniform appearance.
Extrinsic staining typically responds most favourably, with noticeable lightening often achieved within one to two weeks of home tray use or immediately following an in-practice session. Intrinsic stains, particularly those caused by medications or developmental factors, may show more modest improvement and require longer treatment periods or specialised approaches.
Age-related yellowing generally responds well to whitening, though the extent of improvement depends on enamel thickness and the degree of dentine exposure. Teeth with thin enamel may lighten less dramatically than those with thicker, healthier enamel. Existing dental restorations will not change colour, which means careful planning is necessary to achieve a harmonious overall appearance.
Realistic expectations are established during the initial consultation through the use of shade guides, before-and-after photography from previous cases, and honest discussion about probable outcomes. Understanding that whitening is not permanent and that some degree of relapse is natural helps patients make informed decisions about maintenance and long-term care.
Safety and legal clarity are central to professional tooth whitening in the United Kingdom. Regulatory frameworks and professional guidance set clear boundaries for product strength, who may administer treatment, and how it must be delivered.
UK Regulatory Framework:
Products containing or releasing hydrogen peroxide at levels of 0.1% to 6% are regulated and may only be supplied to dental practitioners. Their first application in any cycle must be carried out by a dental practitioner or under the practitioner's direct supervision. Products above permitted limits are restricted. These rules protect patients from harm and ensure clinical oversight where stronger agents are used.
Over-the-counter products legally available to consumers are limited to very low peroxide concentrations, typically 0.1% hydrogen peroxide, which rarely produce a clinically meaningful shade change. For effective whitening with higher peroxide concentrations, a dental assessment and a professionally supplied product are required.
Tooth whitening is recognised in regulatory terms as falling within the practice of dentistry. This means the service should be provided only by appropriately registered professionals working to accepted standards of care. Unregistered or informal whitening services are illegal practices and may be subject to investigation and enforcement.
These principles protect patients and frame ethical practice through informed consent, accurate record-keeping, documented suitability assessment, and documented aftercare. All of these are fundamental elements of compliant, patient-centred whitening services.
Tooth whitening is not a permanent transformation. The longevity of results depends significantly on lifestyle factors and ongoing maintenance. Understanding how to preserve whitening outcomes helps maximise the value of treatment and minimise the frequency of touch-up procedures.
Transient tooth sensitivity is the most common side effect of peroxide-based whitening. Good clinical practice minimises discomfort through the use of desensitising pre-treatment or post-treatment gels where indicated, adjusting wear time and concentration in tray-based regimens, ensuring accurate tray fit to reduce gel contact with gums, and recommending desensitising toothpaste with potassium nitrate or fluoride for daily use.
These measures allow most patients to complete the regimen with minimal interruption. Should sensitivity persist beyond the expected timeframe, consultation with the treating dental professional is advised.
Maintaining whitening results requires a combination of excellent oral hygiene and lifestyle modifications. Strict oral hygiene practices, including thorough brushing and interdental cleaning, help prevent new stain accumulation. Professional cleaning and routine dental reviews allow early detection and management of surface staining before it becomes embedded.
Limiting stain-causing behaviours significantly extends the life of whitening results. Reducing the frequency of coffee, tea, red wine, and tobacco use all contribute to prolonged brightness. When consuming staining beverages, using a straw where practical can reduce direct contact with tooth surfaces.
Touch-up treatments using clinician-prescribed trays or gels can be performed periodically when gradual relapse is noted. Professional polishing and maintenance visits help manage extrinsic staining that develops over time. With appropriate care, many patients enjoy lasting improvement for months to years, with occasional supervised top-ups as required.
Professional whitening begins with a dental assessment and uses clinically suitable products provided by a dental professional. Shop-bought kits are typically limited to low peroxide concentrations and do not replace a full clinical evaluation or the ability to treat intrinsic or restoration-related problems.
When delivered within the current UK regulatory framework by registered professionals, whitening is safe and predictable. Safety hinges on correct assessment, product choice, and adherence to instructions. Temporary sensitivity is common but manageable.
Clinically delivered whitening, at appropriate peroxide concentrations and exposure times, should not cause permanent enamel damage when provided under professional supervision. Excessive or unsupervised use of abrasive home remedies or high-concentration products poses the real risk of enamel erosion.
No. Tooth whitening affects natural tooth structure and will not change the colour of ceramics, composite restorations, or crowns. Any aesthetic plan should discuss the potential need to replace or match restorations after whitening.
Results vary with the method. An in-practice session can produce a noticeable change immediately, while tray-based home systems typically show progressive improvement over one to four weeks, depending on wear time.
Yes. Current guidance restricts the use of products containing or releasing hydrogen peroxide at levels of 0.1% to 6% in those under 18 years, except when used to treat or prevent disease and with appropriate clinical justification.
Tooth whitening is not a routine NHS service and is usually accessed privately. The NHS emphasises that clinician-supplied treatments are the safest and most effective route to whitening.
Contact the dental professional who supplied or supervised the treatment for prompt review and management. Professional care minimises the risk of lasting adverse effects. Ongoing or severe symptoms should be assessed without delay.
Professional tooth whitening has helped countless individuals achieve renewed confidence and satisfaction with their smiles. While individual results vary based on the factors discussed throughout this page, most patients report positive experiences when treatment is delivered with proper assessment, realistic expectations, and appropriate aftercare.
Many patients describe feeling more confident in social and professional situations following whitening treatment. The psychological benefit of an improved smile often extends beyond aesthetics, encouraging better oral hygiene habits and greater attention to overall dental health. This holistic improvement reinforces the value of professional supervision and evidence-based care.
Successful outcomes are characterised not only by the degree of colour change achieved but also by the absence of complications, appropriate management of sensitivity, and patient satisfaction with the naturalness of results. These outcomes are most consistently achieved when treatment follows established clinical protocols and regulatory standards.

Ethical practice forms the foundation of professional tooth whitening. This means providing clear, honest information about realistic outcomes, transparent discussion of limitations, and balanced expectations. Patient-centred consent involves documented informed consent that outlines benefits, likely outcomes, risks, and alternatives.
Clinical record-keeping includes pre-treatment photographs, shade records, and a treatment plan that details product strength and application protocol. Professional whitening avoids over-treatment by recommending whitening only when clinically appropriate and aligning interventions with overall oral health goals. Regulatory compliance ensures that any supply and use of whitening agents meet current legal requirements and professional guidance.
Professional bodies and defence organisations emphasise compliance and patient safety. Dental professionals and regulated team members are expected to follow accepted standards and to report or refuse to participate in unsafe or illegal practice.
Choosing to pursue tooth whitening begins with seeking qualified professional advice. A comprehensive dental assessment determines suitability, identifies any pre-existing conditions requiring attention, and establishes realistic expectations for treatment outcomes.
When selecting a provider, look for demonstrable professional registration and evidence of documented clinical assessment and written treatment plan, use of regulated products and adherence to current guidance about product strengths and supervision, clear before-and-after photography and shade recording, and a practical maintenance plan and accessible aftercare.
Professional regulators and dental defence bodies provide public information about safe practice and record-keeping. Patients are encouraged to verify a clinician's registration status if they have any concerns. The decision to proceed with whitening should be made with full understanding of the process, expected outcomes, and ongoing responsibilities for maintenance.
Professional tooth whitening is grounded in the principle that aesthetic improvement should never compromise oral health. A carefully planned, professionally supervised whitening programme can safely enhance smile brightness, support better oral care habits, and improve confidence.
Legal and clinical frameworks in the United Kingdom are designed to protect patients by ensuring that effective whitening products and procedures are supplied and supervised by qualified dental professionals. Treatment is offered with full assessment, informed consent, and appropriate aftercare.
Understanding the causes of discolouration, the realistic degree of improvement achievable, and the role of dental restorations enables informed decision-making. Professional guidance that emphasises prevention and restoration-aware planning results in better, longer-lasting aesthetic outcomes and greater patient satisfaction.
The public-facing advice from national health services and dental organisations supports prudent, regulated access to whitening so that cosmetic benefit does not come at the cost of oral health. Responsible whitening respects the structural integrity of enamel, acknowledges biological and lifestyle factors, and maintains a commitment to evidence-based, patient-centred care.